The traditional approach to clinical staging has been palpation of the primary tumor as well as inguinal lymph nodes, but this can lead to disease understaging. Multiple imaging modalities are available for more accurate staging, including MRI and PET/CT.
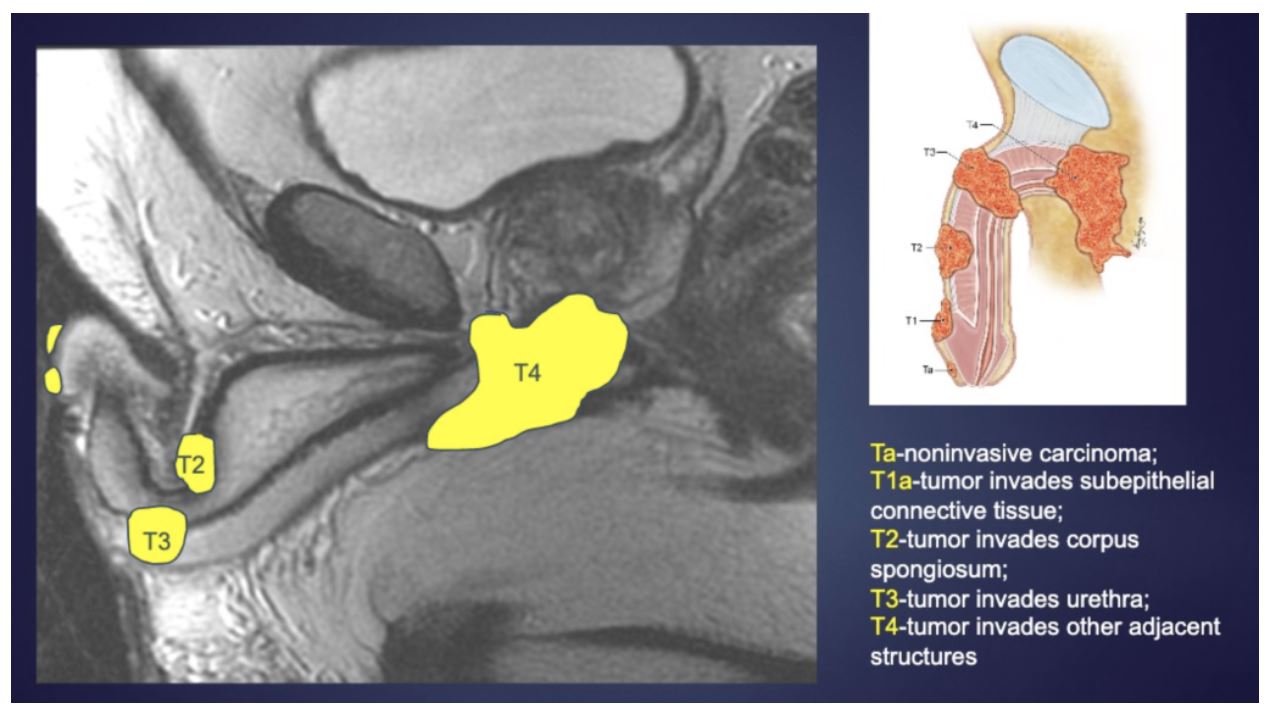
MRI is more accurate than clinical exam for predicting pathologic stage. It has 82% sensitivity and 74% specificity for detection of tunica albuginea invasion, and 63% sensitivity and 82% specificity for detection of urethral invasion. Overall, MRI is accurate 72% of time for predicting pathological stage relative to physical exam (52% accuracy). An example MRI image for staging and associated staging anatomic points is shown below. Overall, MRI is felt to be the best currently available imaging modality for T staging in penile cancer.
What about PET/CT in penile cancer staging? It does not perform as well for T stage due to poor localization relative to adjacent anatomical structures, though this could be improved with getting iodinated contrast and diagnostic level CT imaging. However, the SUVmax of a tumor does seem to reflect tumor infiltration of connective tissue as well as adjacent blood vessels and lymphatics as well as poor differentiation status. Available data suggests an SUVmax threshold of 16.6 is capable of stratifying patients by cancer specific survival, though this number may vary by PET scanner.

With regards to detection of lymph node involvement in patients with no clinically palpable adenopathy, both MRI and PET/CT can be used. PET/CT can also be used to detect distant metastatic disease beyond the typical locoregional lymph node spread of penile cancer.

MRI is more accurate than clinical exam for predicting pathologic stage. It has 82% sensitivity and 74% specificity for detection of tunica albuginea invasion, and 63% sensitivity and 82% specificity for detection of urethral invasion. Overall, MRI is accurate 72% of time for predicting pathological stage relative to physical exam (52% accuracy). An example MRI image for staging and associated staging anatomic points is shown below. Overall, MRI is felt to be the best currently available imaging modality for T staging in penile cancer.

What about PET/CT in penile cancer staging? It does not perform as well for T stage due to poor localization relative to adjacent anatomical structures, though this could be improved with getting iodinated contrast and diagnostic level CT imaging. However, the SUVmax of a tumor does seem to reflect tumor infiltration of connective tissue as well as adjacent blood vessels and lymphatics as well as poor differentiation status. Available data suggests an SUVmax threshold of 16.6 is capable of stratifying patients by cancer specific survival, though this number may vary by PET scanner.

With regards to detection of lymph node involvement in patients with no clinically palpable adenopathy, both MRI and PET/CT can be used. PET/CT can also be used to detect distant metastatic disease beyond the typical locoregional lymph node spread of penile cancer.

In one small study, MRI accurately staged 13 out of 15 patients whereas clinical exam was accurate in less than half of the cases. PET/CT was found to have a high sensitivity (81%) and specificity (92%) across 41 patients in a study, but when looking at only clinically node negative patients, the sensitivity and specificity dropped to 57% and 86% respectively. Given its high specificity, PET/CT can be used to further evaluate lymph nodes for evidence of elevated SUV suggestive of cancer in cases where it would be advisable to avoid surgery if negative (patient with comorbidities or otherwise unresectable inguinal disease). It can also be used to follow-up on treatment effect from primary chemotherapy or radiation therapy.
MRI-PET fusion may result in the best of both worlds, accurate T staging as well as assessment for distant metastatic disease. This is not widely available but may benefit from further investigation.
In conclusion, the presenter summarized that MRI is most helpful with local staging whereas PET/CT is helpful for assessment in distant disease or potentially avoiding surgery in patients who may have adverse surgical outcomes. Additionally, SUVmax may help predict overall prognosis though this has not been evaluated in larger cohorts of patients.
Presented by: Priya Bhosale MD, Professor of Radiology, University of Texas MD Anderson Cancer Center, Houston, Texas
Written by: Alok Tewari, MD, PhD, Medical Oncology Fellow at the Dana-Farber Cancer Institute, at the 2020 Genitourinary Cancers Symposium, ASCO GU #GU20, February 13-15, 2020, San Francisco, California
MRI-PET fusion may result in the best of both worlds, accurate T staging as well as assessment for distant metastatic disease. This is not widely available but may benefit from further investigation.
In conclusion, the presenter summarized that MRI is most helpful with local staging whereas PET/CT is helpful for assessment in distant disease or potentially avoiding surgery in patients who may have adverse surgical outcomes. Additionally, SUVmax may help predict overall prognosis though this has not been evaluated in larger cohorts of patients.
Presented by: Priya Bhosale MD, Professor of Radiology, University of Texas MD Anderson Cancer Center, Houston, Texas
Written by: Alok Tewari, MD, PhD, Medical Oncology Fellow at the Dana-Farber Cancer Institute, at the 2020 Genitourinary Cancers Symposium, ASCO GU #GU20, February 13-15, 2020, San Francisco, California

