In an effort to address this on a larger scale, the authors of this study combined the results of 9 randomized phase III trials. As we all know, most clinical trials often underrepresent minority populations, including African-Americans. They started with 15 trials total, and ended up with 10 phase III trials – since one was unavailable for data analysis, they analyzed 9 remaining trials. By combining all 9 trials, the hope was that small sample size limitations could be overcome. Ultimately, this was an ad-hoc analysis and not actually powered for this specific question.
The 9 trials are:
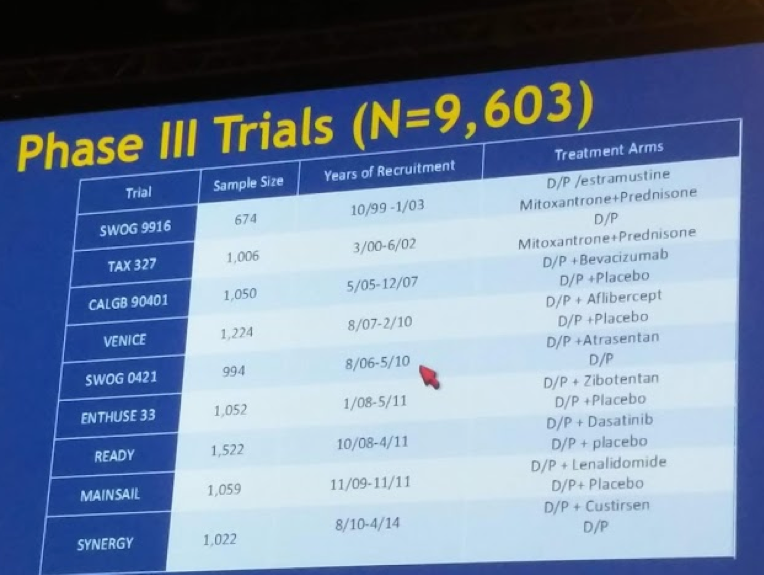
The primary goal of this analysis was to compare OS in AA men to Caucasian men treated with docetaxel/prednisone or a docetaxel/prednisone-containing regimen. Individual patient data from 8,871 mCRPC men randomized on nine phase III trials to docetaxel/prednisone (DP) or a DP containing regimen were combined. Race used in the analysis was based on self-report.
The primary endpoint was OS, defined as the time between randomization and death or date of last follow-up if patients were alive. Adjusting for established risk factors that were common across the trials (age, PSA, performance status, alkaline phosphatase, hemoglobin, and sites of metastases), a proportional hazards model was used to assess the prognostic importance of race (AA vs. C).
Of 8,871 patients, 7,528 (85%) were C, 500 (6%) were AA, 424 were Asian (5%) and 419 (4%) had race unspecified. This highlights the severe underrepresentation of minorities in these studies, especially considering the changing demographics of the United States. With the US expected to be a majority minority population in the next few decades, clinical trials need to change to reflect that. For this analysis, the last two groups were deleted from the analysis leaving 8,452 pts.
Looking specifically at the AA representation in each trial and separated by US/NCTN studies vs. Industry/international trials:
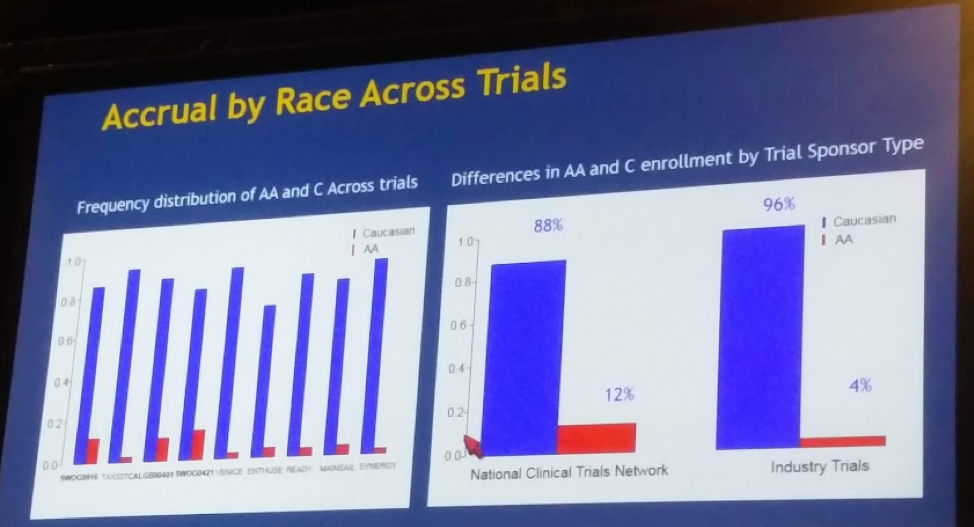
The NCTN trials were more representative, with 12% inclusion. Current US demographics put AA population at 15%.
Baseline demographics of the cohort were as follows:
Median age was 69 years and 94% had performance status 0-1. Median hemoglobin, PSA, and alkaline phosphatase were 12.9 g/dL, 86 ng/mL and 139 U/L, respectively. The pattern of metastatic spread was: 72% bone disease with or without lymph nodes, 9% lung disease, 9% liver disease and 7% lymph nodes only.
- Comparing AA to C, baseline characteristics were mostly similar
- AA men were slightly younger (67.6 vs. 69)
- AA men had a higher baseline PSA (127 vs. 85)
Based on this, it would appear that there was a statistically significant increased OS in African-American men vs. Caucasian men with mCRPC who were eligible to be enrolled on these clinical trials. However, as this is a small population of AA men who were well selected, further understanding the biological variation by race in men with mCRPC treated with DP is warranted.
Selection criteria may have influenced outcomes.
One important take-away is that while the NCTN is doing a good job recruiting minority men, there is still a significant gap between trial enrollment ratios and actual population proportions.
Presented by: Susan Halabi, Ph.D., FASCO, Duke University Medical Center
Co-Authors: Sandipan Dutta, Catherine M. Tangen, Mark Rosenthal, Daniel Peter Petrylak, Ian Murchie Thompson, Kim N. Chi, Johann S. De Bono, Abderrahim Fandi, John C. Araujo, Mario A. Eisenberger, Christopher Logothetis, David I. Quinn, Karim Fizazi, Celestia S. Higano, Daniel J. George, Michael J. Morris, Eric Jay Small, Ian Tannock, William Kevin Kelly
Author Information: Duke University Medical Center, Durham, NC; Duke University, Durham, NC; Fred Hutchinson Cancer Research Center, Seattle, WA; The Royal Melbourne Hospital, Parkville, Australia; Yale School of Medicine, New Haven, CT; UT Health Science Center, San Antonio, TX; British Columbia Cancer Agency - Vancouver Centre, Vancouver, BC, Canada; The Institute of Cancer Research and The Royal Marsden NHS Foundation Trust, Sutton, United Kingdom; Celgene, Summit, NJ; The University of Texas MD Anderson Cancer Center, Houston, TX; The Sidney Kimmel Comprehensive Cancer Center at Johns Hopkins University, Baltimore, MD; University of Texas MD Anderson Cancer Center, Houston, TX; University of Southern California Norris Comprehensive Cancer Center, Los Angeles, CA; Gustave Roussy, Villejuif, France; University of Washington and Fred Hutchinson Cancer Research Center, Seattle, WA; Memorial Sloan Kettering Cancer Center, New York, NY; University of California San Francisco, San Francisco, CA; Princess Margaret Cancer Centre, University of Toronto, Toronto, ON, Canada; Sidney Kimmel Cancer Center at Thomas Jefferson University, Philadelphia, PA
Written by: Thenappan Chandrasekar, MD, Clinical Fellow, University of Toronto, twitter: @tchandra_uromd at the 2018 ASCO Annual Meeting - June 1-5, 2018 – Chicago, IL USA

