(UroToday.com) The 2022 Advanced Prostate Cancer Consensus Conference (APCCC) Hybrid Meeting included a session on the management of metastatic hormone sensitive prostate cancer (mHSPC) and a presentation by Dr. Mary Ellen Taplin discussing systemic treatment options for different subgroups among patients with mHSPC. Dr. Taplin notes that the actual number of M0 M1 versus de novo mHSPC patients is likely a function of (i) PSA screening and treatment of localized disease (ie. higher in the USA than in the UK), and (ii) treatment with ADT for rising PSA after local therapy leading to M0 CRPC. Furthermore, many men with M0 to M1 HSPC may get SBRT and not get referred for trials and put on intermittent ADT. As follows is mHSPC in the disease continuum:

Based on SWOG, MD Anderson Cancer Center, CHAARTED, and LATITUDE data, Dr. Taplin highlighted the following mHSPC prognostic groups based on the distribution of metastases:

Different prognoses are noted by type of presentation and extent of metastases based on CHAARTED and GETUG-15:
- Metachronous and low volume: median OS ~8 years
- Metachronous and high volume: median OS 4.5 years
- Synchronous and low volume: median OS 4.5 years
- Synchronous and high volume: median OS 3 years
Over the last several years, the mHSPC disease space has been defined by testosterone suppression plus: (i) chemotherapy, (ii) androgen synthesis inhibitor, (iii) potent androgen receptor inhibitor, (iv) radiation to the primary prostate tumor, or (v) potent antiandrogen + chemotherapy (triple therapy:

Dr. Taplin then discussed the PEACE-1 trial that was recent published in Lancet.1 Men with mHSPC were randomly assigned (1:1:1:1) to standard of care (ADT alone or with intravenous docetaxel 75 mg/m2 once every 3 weeks), standard of care plus radiotherapy, standard of care plus abiraterone (oral 1000 mg abiraterone once daily plus oral 5 mg prednisone twice daily), or standard of care plus radiotherapy plus abiraterone. There were 1,173 patients randomized, with a median follow-up was 3.5 years (IQR 2.8–4.6) for radiographic progression-free survival and 4.4 years (3.5–5.4) for overall survival. In the overall population, patients assigned to receive abiraterone (n=583) had longer radiographic progression-free survival (HR 0.54, 99.9% CI 0.41–0.71) and overall survival (0.82, 95.1% CI 0.69–0.98) than patients who did not receive abiraterone (n=589):
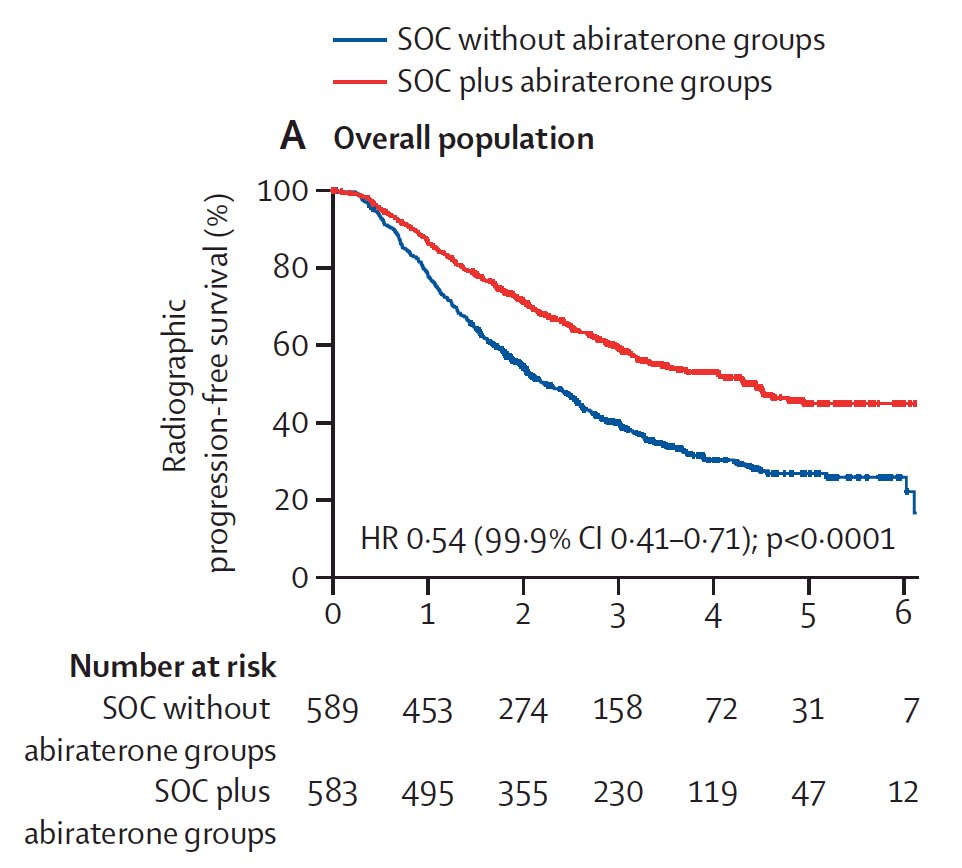
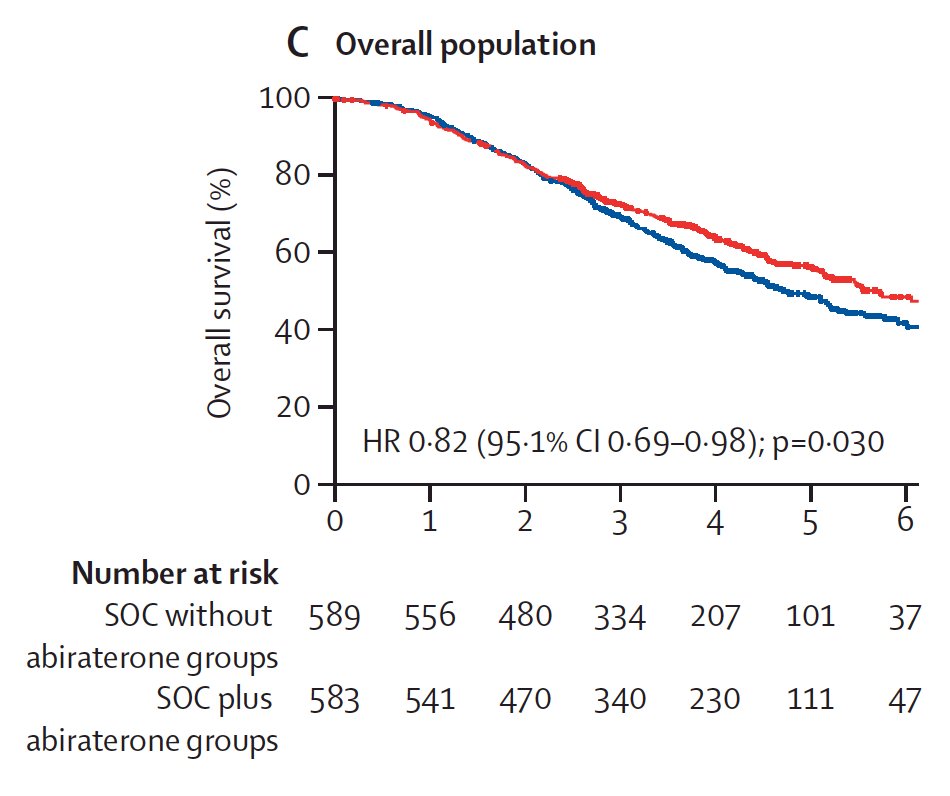
In the ADT with docetaxel population (n=355 in both with abiraterone and without abiraterone groups), the HRs were consistent (radiographic progression-free survival 0.50, 99.9% CI 0.34–0.71; overall survival 0.75, 95.1% CI 0.59–0.95). Importantly, this benefit was consistent across multiple subgroups.
Dr. Taplin’s conclusions from the PEACE-1 trial are as follows:
- Adding abiraterone to ADT + docetaxel significantly improves rPFS by 2.5 years in men with de novo prostate cancer
- Overall survival also improved with a 25% reduction in the risk of death, even when mCRPC men in the control group received at least one life-prolonging treatment
- This benefit translates to a median lifetime gain of more than 1.5 years for men with high volume metastases (5.1 vs 3.5 years); OS data for low volume men may be immature
- Toxicity was as expected, with no apparent synergistic side effects from this combination
In the phase 3 ARASENS trial, 1,306 men with metastatic, hormone-sensitive prostate cancer were randomized 1:1 to receive darolutamide (at a dose of 600 mg [two 300-mg tablets] twice daily) or matching placebo, both in combination with ADT and docetaxel. The risk of death was significantly lower, by 32.5%, in the darolutamide group than in the placebo group (HR 0.68, 95% CI 0.57 to 0.80):

Darolutamide was also associated with consistent benefits with respect to the secondary endpoints and prespecified subgroups, including time to castration-resistant prostate cancer (HR 0.36, 95% CI 0.30-0.42):

And time to pain progression (HR 0.79, 95% CI 0.66-0.95):
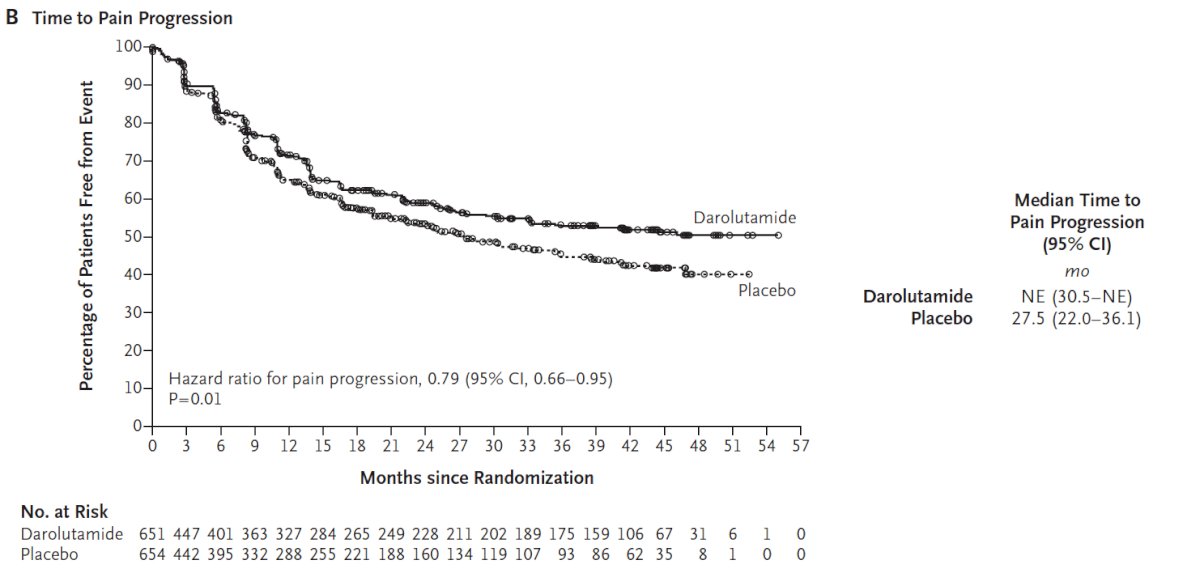
With the progression from ADT alone to doublet therapy to triplet therapy, there has been a progressive increase in median OS for patients with de novo high volume mHSPC, as highlighted in the following figure:
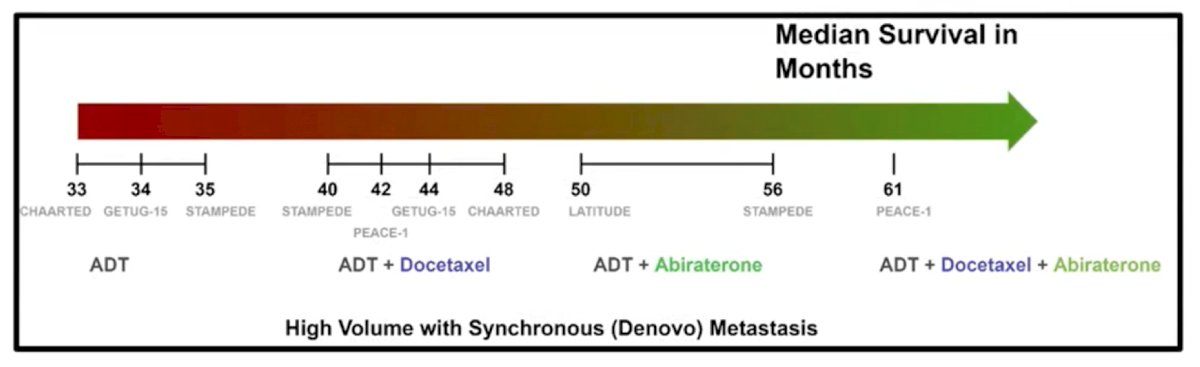
Dr. Taplin notes that there are several gray areas that remain among men with mHSPC, including (i) the influence of chemotherapy versus NHT in mHSPC (currently, there are no active phase 3 trials), and (ii) outcomes in low volume disease defined by PSMA-PET with negative conventional imaging.
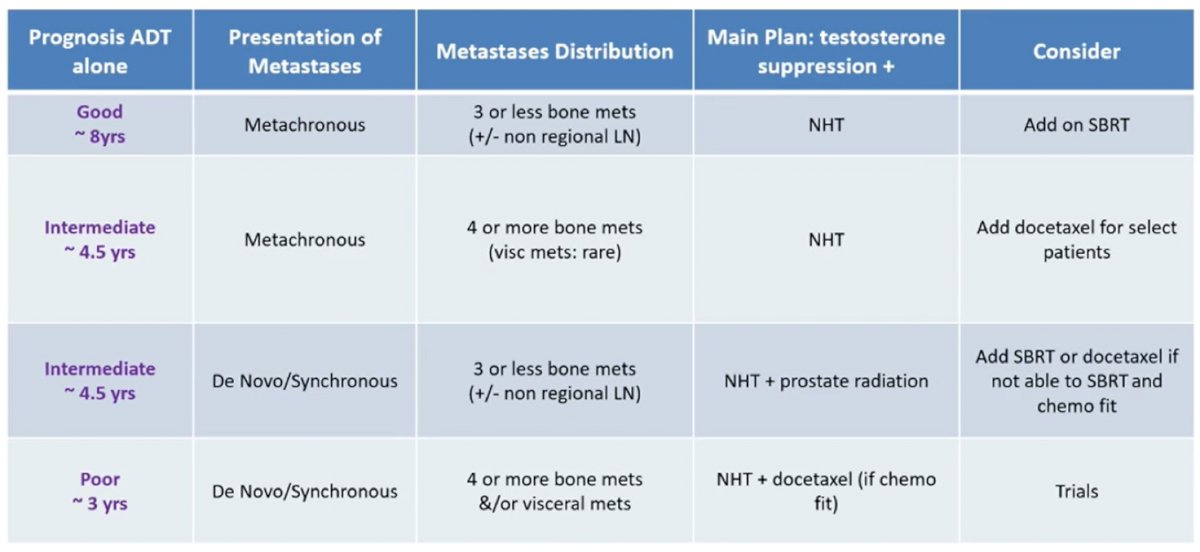
Dr. Taplin concluded her presentation by discussing systemic treatment options for different subgroups of patients with mHSPC with the following summary table of mHSPC treatment plans by risk groups:
Presented by: Mary Ellen Taplin, MD, Dana-Farber Cancer Institute, Harvard Medical School, Boston, MA
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2022 Advanced Prostate Cancer Consensus Conference (APCCC) Annual Hybrid Meeting, Lugano, Switzerland, Thurs, Apr 28 – Sat, Apr 30, 2022.
References:
- Fizazi K, Foulon S, Carles J, Roubaud G, et al. Abiraterone plus prednisone added to androgen deprivation therapy and docetaxel in de novo metastatic castration-sensitive prostate cancer (PEACE-1): A multicentre, open-label, randomized, phase 3 study with a 2 x 2 factorial design. Lancet. 2022 Apr 30;399(10336):1695-1707.
- Smith MR, Hussain M, Saad F, et al. Darolutamide and Survival in Metastatic, Hormone-Sensitive Prostate Cancer. N Engl J Med. 2022 Mar 24;386(12):1132-1142.

