Data show that 25% of GGG2 were actually GGG>=3 at radical prostatectomy (under-graded).1 Unfortunately, there is no criteria to identify true low risk in low volume intermediate risk. In a study assessing AS in the Goeteborg Prostate Cancer Screening trial, 104/474 patients had intermediate risk PC, accounting for 83% of the patients with cancer-specific mortality. Approximately 80% of these intermediate-risk patients were GGG2, and the hazard ratio for failure for intermediate risk vs. very low risk was 4.8 (Figure 1).2
Figure 1 – Failure-free survival according to NCCN risk group:
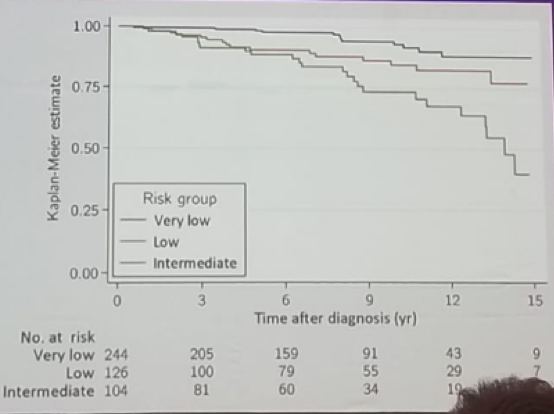
In the PROTECT study, 77% of the patients were Gleason 6 on biopsy. Only 120 men in each group were with Gleason 7 or higher.3 This study was underpowered to show a difference and results are misleading in this regard, according to Dr. Klotz.
Dr. Klotz then discussed the question whether MRI and novel biomarkers will transform this controversy of AS in IRPC. The answer is most probably yes, but neither MRI and the novel biomarkers are perfect. With GGG1 disease, the goal of monitoring is to identify the presence of higher grade cancer. With GGG2 disease, triggers for intervention are not so obvious, and metastasis may occur during the surveillance period. We cannot be 100% certain that a Gleason 3+4 disease with a stable MRI lesion does not metastasize during surveillance. Various studies have shown that MRI has a negative predictive value of ruling out clinically significant cancer between 76%-100% as summarized in Table 1.
Dr. Klotz summarized his excellent talk and reiterated that all studies of Gleason 7 on AS show substantially increased risk of metastasis with long term follow-up (despite offering selective delayed intervention). Many patients do well, but the risk is substantial and not to be taken lightly. The key has always been and will remain patient selection and identification of relevant triggers.
There are many emerging therapeutic alternatives – focal therapy (HIFU, Cryotherapy, Brachytherapy, electroporation, and more), which are being incorporated into the standard of care and their exact role will need to be sorted out in the future. Lastly, MRI and biomarkers have limitations, and validation in this setting is mandatory.
Table 1: How well does MRI detect and rule out clinically significant cancer?
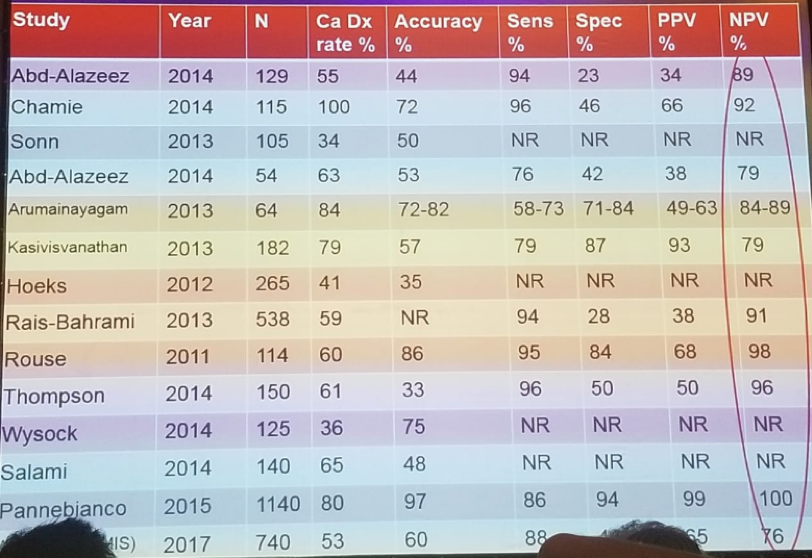
References:
1. Patel HD, Jama Onc. 2018
2. Godtman RA Eur Urol 2016
3. Hamdy FC et al. NEJM 2016
Presented by: Laurence Klotz, MD, Sunnybrook Health Science center, Toronto, Ontario, Canada
Written by: Hanan Goldberg, MD, Urologic Oncology Fellow (SUO), University of Toronto, Princess Margaret Cancer Centre @GoldbergHanan at the 2018 FOIU 4th Friends of Israel Urological Symposium, July 3-5. 2018, Tel-Aviv, Israel
Read the Opposing Argument: Active Surveillance for Intermediate Risk Prostate Cancer - FOR

