The encouraging surgical results presented in this report, i.e. 82% able to achieve or resume satisfactory erections vs. 9% prior to the procedure, stand on three feet:
- Pharmacologically-challenged penile duplex sonography (PC-PDS)
- Pharmacologically-challenged computed caverno-tomography (PC-CCT)
- An innovative combination of open and endovascular surgery.
Several observations can be made from this experience. A standardized PC-PDS methodology is required to identify patients who may actually benefit from this complex surgery, i.e. with actual leakage. A strong-enough pharmacological stimulation avoids false positives. Leakages should be assessed directly on veins themselves, not only based on End Diastolic Velocity indirect criteria.
PC-CCT with a similar pharmacologically stimulation as for PC-PDS and 3D reconstructions allow for preoperative planning according to leakage patterns. This personalized planning reduces failures due to incomplete neutralization of leakages. Surgery of CVLs requires a combination of open and endovascular techniques, not mere deep dorsal vein ligations or embolizations. This surgery may be regarded as complex, but the closing of leakages and of veins to be recruited when intra-cavernosal pressure will raise is key. Per-operative penile and vascular imaging using a hybrid room allows for precise endovascular targeting of leaks and assessment of results to ensure maximum completeness of surgery.
Selection among patients with CVL of those who may best benefit from surgery is another important issue. Surprisingly, results were similar in younger and older patients, with primary or secondary ED, and diabetes did not have a negative impact on results. Yet, patients were proposed CVL surgery only if arterial and neurological diseases were absent or light, after a pre-operative work-up assessing arterial and hormonal status, penile electromyography if required. As a consequence, results represent surgery on pure CVLs, excluding to the maximum other components of ED.
Quality control with a three-month post-operative PC-PDS using a standardized protocol allows for documenting the actual contribution of CVL to ED. In other words, CVLs can be efficiently identified with adequate PC-PDS criteria assessing penile venous flow directly, and surgery improves patient erections as well as hemodynamic parameters.
These results require confirmation with higher numbers and from other groups applying similar pre-operative workup and operative techniques. Future directions include exploring whether this surgery can be proposed to patients with milder albeit disabling ED, and the identification of causes of failure. One site of CVL unknown until now has been identified from this experience, i.e. the crus region of the corpora cavernosa (Figures 1 and 2), and caverno-spongious shunts appear to play a more than expected role in CVLs, both of them hampering surgical results when ignored.
Patients with CVL and resistance to PDE-5I with sufficient arterial inflow and normal neurological stimulation could benefit from this improved approach. By reducing venous outflow, overall rigidity is improved. It becomes an option for patients who do not respond to medical treatment and are reluctant to accept an implant, and to young patients with primary dysfunction.
The authors thank Claude Schulman, Professor Emeritus of Urology, Bruxelles, Belgium, for his constructive reading of the manuscript.

Figure 1. Ultrasound of the crus region of the left corpus cavernosum. The white arrow points to venous leakage in blue.
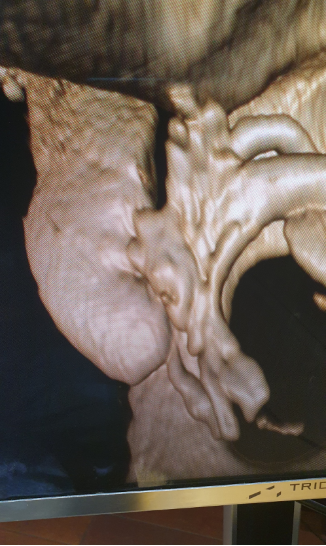
Figure 2. Computed caverno-tomography from the same patient confirms the leak of the crus region of corpus cavernosum CC).
Written by: Eric Allaire, MD, PhD, Hélène Sussman, MD, Ronald Virag, MD, Centre d’Explorations et Traitements de l’Impuissance (CETI), Paris, France
Read the Abstract

