(UroToday.com) The Society of Urologic Oncology (SUO) 2021 annual meeting in Orlando, FL hosted a second State of the Art Lecture by Dr. Robert Dreicer, MD, MS, MACP, FASCO discussing adjuvant therapy for kidney cancer.
Dr. Dreicer began his talk by giving a case presentation of one of his former patients from 1989. This was a 44-year-old farmer who presented with worsening abdominal pain and gross hematuria, subsequently found to have a 16 cm right renal mass without evidence of metastasis, Hgb 7.8. Chest imaging was negative, and the patient subsequently underwent an open radical nephrectomy with final pathology demonstrating high-grade clear cell renal cell carcinoma (RCC). This patient was referred to Dr. Dreicer 3.5 months post-operatively for consideration of adjuvant treatment given his high risk of disease recurrence. Unfortunately, at that time, there were no adjuvant treatment options for that patient.
Dr. Dreicer next defined adjuvant therapy as that given after primary treatment to lower the risk of cancer recurrence. He went on to detail the “metaphysics” behind adjuvant therapy:
- Historically “active” agents have been moved up from the metastatic setting into the adjuvant setting
- Duration of therapy: combination of pragmatism and safety/tolerability
- Practical issues: who manages the care of the patient in the long term
- Intangibles: emotional need to help patients with likely bad outcomes
- Realities: No matter how effective adjuvant therapy is, we are treating some patients who are already cured
With regards to RCC:
- 65% of patients present with localized disease and 16% with locoregional disease
- 40-50% of patients are potentially at risk of developing metastatic disease
- Standard of care remained observation for a long time
- Sunitinib’s Food and Drug Association (FDA) approval in the adjuvant setting in 2017 has not resulted in a significant uptake in clinical practice
The first adjuvant trials in the RCC setting evaluated interferon (IFN), with a trial of 294 patients receiving 9 months of IFN versus placebo having no overall survival (OS) benefit. A subsequent trial randomized patients to IFN for six months versus observation, again with no OS benefit. Subsequently, Interleukin-2 (IL-2) was evaluated, again with no OS benefit. Combination trials of IL-2 and IFN were similarly negative for OS benefit.
Adjuvant trials of tyrosine kinase inhibitors (TKIs): ASSURE, PROTECT, and ATLAS were all negative trials. S-TRAC, a randomized, double-blind, phase 3 trial of 615 patients with locoregional, high-risk clear cell RCC randomized to receive either sunitinib 50 mg every day or placebo on a 4-weeks-on, 2-weeks-off schedule for one year or until disease recurrence demonstrated a disease-free survival (DFS) benefit from 5.6 years in the placebo arm to 6.8 years in the sunitinib arm (HR 0.76, p=0.03). Notably, the ASSURE trial, which also included sunitinib, was a negative trial. The adverse event profile of sunitinib in both trials was ~60% with many patients averse to taking this medication in the metastatic setting, let alone the adjuvant setting.1,2
Does this data translate to the metastatic, no evidence of residual disease (M1NED) space? Multiple retrospective series have reported a benefit compared to alternative management from the pre-immunotherapy era. A randomized phase three trial of one year “adjuvant” pazopanib versus surveillance following metastasectomy paradoxically demonstrated a superior OS in the placebo arm (HR 2.65), clearly proving the futility of this approach.3
This brings us to the KEYNOTE-564 trial that evaluated adjuvant pembrolizumab after nephrectomy in RCC patients. The key eligibility criteria and study design/objectives are illustrated in the image below. Patients were risk-stratified into intermediate-high (86% of total), high (8%), and M1NED risk (6%) subgroups.
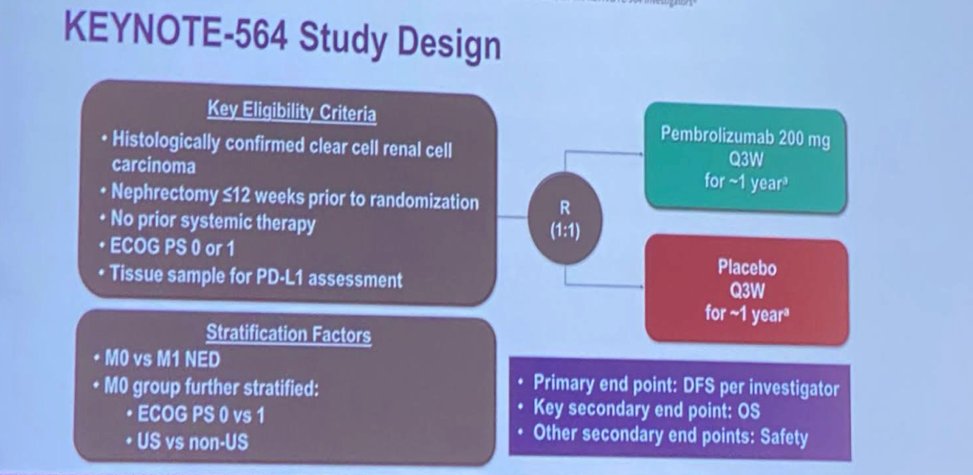
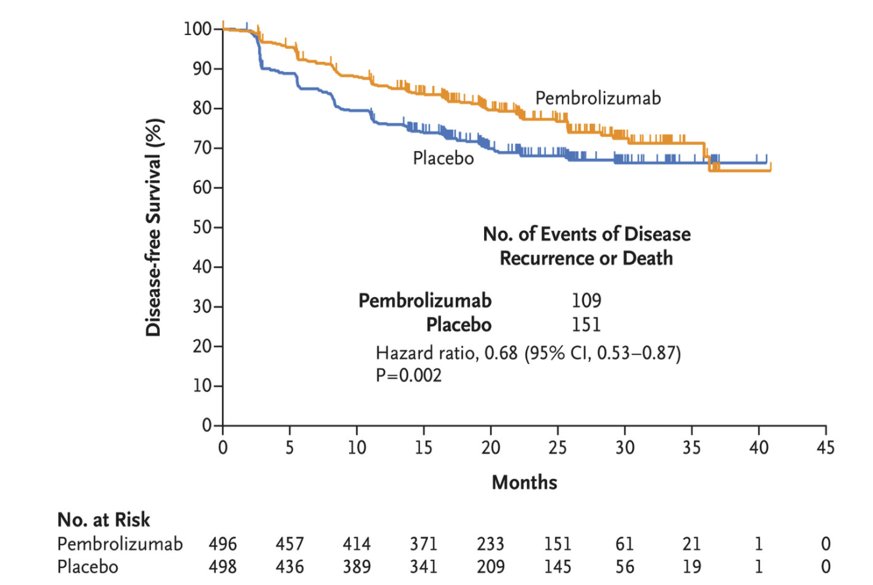
DFS at 24 months was 77% in the pembrolizumab arm compared to 68% in the placebo arm. Twenty percent of patients receiving pembrolizumab had serious adverse reactions with two therapy-related deaths. The discontinuation rate secondary to toxicity (elevated liver function tests, colitis, adrenal insufficiency) was 21%. Twenty-six percent of patients had dose interruptions. As has been previously documented, the FDA granted approval for this drug on November 17, 2021.
What were the strengths and limitations of this study, per Dr. Drecier?
- Broad range of risk groups enrolled
- Enriched for Programmed Death Ligand (PD-L1) positive patients
- Blinded investigator-assessed endpoints
- Deaths without tumor progression were not censored thus potentially overestimating DFS
- Pembrolizumab activity was observed across prespecified subgroups and agnostic of PD-L1 expression
- At time of presentation only 26% of deaths were needed for final analysis of OS but with a questionable signal
Next, Dr. Dreicer summarized the four ongoing adjuvant/perioperative immune checkpoint trials in this disease space.

Dr. Dreicer went on to elaborate on the need for markers to predict response to adjuvant therapy with RCC. He drew parallels from the muscle-invasive bladder cancer disease space, whereby although the CheckMate-274 trial demonstrated an OS benefit for adjuvant nivolumab,4 the IMvigor010 trial of adjuvant atezolizumab did not meet its primary endpoint of DFS in the intention to treat population.5 Post-hoc analysis using circulating tumor DNA (cTDNA) however demonstrated that ctDNA positive patients had improved DFS and OS with atezolizumab, clearly discerning a subset of patients to target despite the overall negative results.6
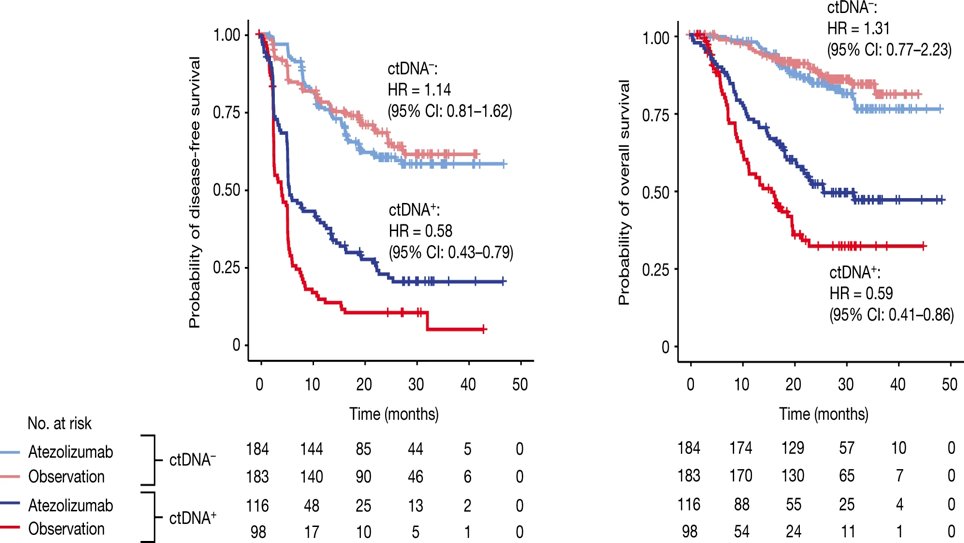
What is the value of ctDNA in RCC?
- crDNA levels in patients with metastatic clear cell RCC higher than healthy volunteers and benign lesions
- ctDNA levels can correlate with tumor stage, grade, and metastatic disease
- Disease burden was found to be directly correlated with detectable ctDNA
- Several studies however show that only 30% of RCC patients had detectable ctDNA mutations, even in genes previously described to be associated with RCC→ RCC is a low shedding tumor
Dr. Dreicer concluded his talk with the following take-home messages:
- Recent therapeutic developments have led to improvement in outcomes in a relatively small subset of patients with metastatic RCC
- Data from KEYNOTE-564 is provocative and for the highest risk patients this approach appears supported and is now FDA approved
- Ultimately will need to understand both who needs to be treated and, of those, who are likely to derive treatment benefit
- If adjuvant immune checkpoint inhibitors become a “standard of care” there will be important ramifications for management of metastatic RCC
Presented by: Robert Dreicer, MD, MS, MACP, FASCO, Head, Medical Oncology Section, Deputy Director University of Virginia Comprehensive Cancer Center, Associate Director for Clinical Research, Co-Director Paul Mellon Urologic Oncology Center, Professor of Medicine and Urology, University of Virginia School of Medicine, Charlottesville, VA
Written by: Rashid Sayyid, MD, MSc – Urology Chief Resident, Augusta University/Medical College of Georgia, @rksayyid on Twitter during the 2021 Society of Urologic Oncology (SUO) Winter Annual Meeting, Orlando, FL, Wed, Dec 1 – Fri, Dec 3, 2021.
References:
- Ravaud A, Motzer RJ, Pandha HS, et al. Adjuvant Sunitinib in High-Risk Renal-Cell Carcinoma after Nephrectomy. N Engl J Med 2016;375(23):2246-2254.
- Haas NB, Manola J, Uzzo RG, et al. Adjuvant sunitinib or sorafenib for high-risk, non-metastatic renal-cell carcinoma (ECOG-ACRIN E2805): A double-blind, placebo-controlled, randomised, phase 3 trial. Lancet 2016;387(10032):2008-2016.
- Appleman LJ, Puligandla M, Pal SK, et al. Randomized, double-blind phase III study of pazopanib versus placebo in patients with metastatic renal cell carcinoma who have no evidence of disease following metastasectomy: A trial of the ECOG-ACRIN cancer research group (E2810). J Clin Oncol. 2019.
- Bajorin DF, Witjes JA, Gschwend JE, et al. Adjuvant nivolumab versus placebo in muscle-invasive urothelial carcinoma. N Engl J Med. 2021 Jun 3;384(22):2102-2114.
- Bellmunt J, Hussain M, Gschwend JE, et al. Adjuvant atezolizumab versus observation in muscle-invasive urothelial carcinoma (IMvigor010): A multicentre, open-label, randomized, phase 3 trial. Lancet Oncol. 2021 Apr;22(4):525-537.
- Powles T, Assaf ZJ, Davarpanah N, et al. ctDNA guiding adjuvant immunotherapy in urothelial carcinoma. Nature. 2021 jul;595(7867):432-437.

