Dr. Ingels began with a case presentation of a 71-year-old man seen with respect to an elevated prostate-specific antigen (PSA) of 14.96 ng/mL in the context of a prior negative biopsy 8 years prior. The digital rectal examination demonstrated no nodule. In terms of past medical history, he was an active smoker with a history of benign prostatic hyperplasia (BPH) and hypertension, treated with alfuzosin and hydrochlorothiazide (HCTZ), respectively.
Further investigation was performed with mpMRI which demonstrated a 97 mL gland with three PIRADS4 nodules, ranging from 5 to 12 mm. Prostate biopsy was then performed with a standard 12 core template in addition to 6 targeted cores. Two of these were positive with evidence of Gleason 4+3 disease. This gentleman then underwent conventional staging imaging with a bone scan which was negative and a computed tomography scan which demonstrated a 12mm pelvic nodule and multiple small (<10mm) lymph nodes. As a result of these CT findings, the patient underwent PSMA PET-CT which demonstrated two suspicious lesions, one in the left peri-vesical region (SUV 3.9) and one in the right distal external iliac chain (SUV 4.4).
Dr. Eden then presented, arguing that the PSMA PET-CT would influence the role of PLND. Dr. Eden began by highlighting the EAU prostate cancer guidelines which recommend the use of extended nodal dissection for patients with a risk of nodal metastasis that exceeds 5%. Doing so means that 94% of patients will be correctly staged. Dr. Eden highlighted that there is a spectrum of nodal involvement ranging from complete replacement to microscopic foci of disease.
Dr. Eden postulates that we are currently towards the end of the era of pelvic lymphadenectomy being performed as a staging procedure, suggesting instead that advanced imaging can fulfill this staging role. To this end, he emphasized three reasons, that PNLD:
- is responsible for more of the morbidity of radical prostatectomy
- does not improve survival
- has non-invasive alternatives, namely PSMA PET-CT.
Dr. Eden then discussed the potential oncologic benefits of node dissection, emphasizing that iliac artery and obturator fossa dissection is inadequate. Historical data suggest that excision of at least 4 lymph nodes (or more than 10 nodes in those who were node-negative) is associated with improved cancer-specific survival, compared to those who did not undergo node dissection. These data have driven high volume lymphadenectomy in many centers. Dr. Eden highlighted further data showing that the number of lymph nodes removed correlates with prostate cancer-specific survival. However, he emphasized that systematic reviews have highlighted that there is a high risk of bias and confounding, and conflicting results between studies without consistent benefits in terms of survival.
In synthesizing the data, he highlighted that PLND is a morbid procedure without evidence of oncologic benefits. Dr. Eden views the future as non-invasive staging using PSMA PET-CT. Notably, he highlighted that current data suggest that the specificity of PSMA PET-CT is similar to the accuracy of staging by lymphadenectomy cited in guidelines. Further, nearly 50% of men have metastases outside of the lymphadenectomy template, thus increasing the value of this approach.
In conclusion, Dr. Eden suggested that extended pelvic lymphadenectomy should no longer be considered the standard of care for nodal staging. For patients undergoing PSMA PET-CT, he suggested that it is reasonable to remove PET-avid nodes to confirm involvement and as part of a debulking multi-modality approach.
Dr. Briganti then presented an alternative approach. He began by discussing what he called certainties in imaging for nodal staging in prostate cancer:
- PSMA PET-CT is more accurate than conventional imaging.
- PSMA PET-CT is more specific than conventional imaging in patients with suspicious lymph nodes.
- PSMA PET-CT can miss micro-metastatic disease.
- PSMA PET-CT changes the template of extended pelvic lymph node dissection in some cases.
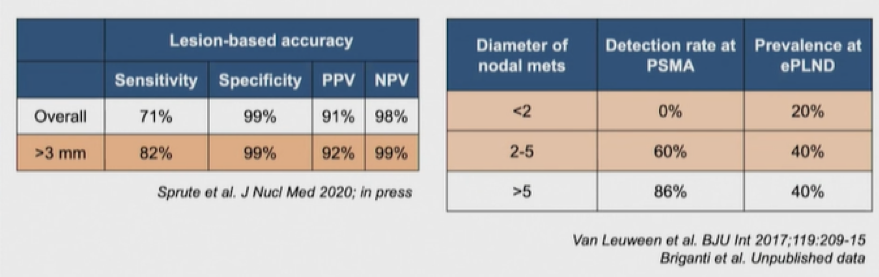
Dr. Briganti highlighted data for the sensitivity of PSMA PET-CT, emphasizing that there are limitations in the sensitivity of this approach. While earlier data suggested a sensitivity of approximately 75%, Dr. Briganti suggested that more recent data are closer to 50%, on a per-patient and per node/template analysis.
This is, in Dr. Briganti’s view, as a result of the presence of micro-metastatic disease, which may account for up to 60% of patients and is often missed by PSMA PET-CT.
Dr. Briganti then assumed that, based on the ProPSMA trial, there will be a change to the routine use of PSMA PET-CT for upfront staging of all intermediate and high-risk patients. On this basis, there will be three scenarios in his view, in each case, he argued that clinical management will not change:

Addressing the first of those scenarios, he felt that we could not avoid PLND in patients with a negative PSMA PET-CT, based on the negative predictive values which may be as low as 67% (and decrease with an increasing prevalence of nodal involvement).
In the case of oligometastatic disease on the basis of PSMA PET-CT, it is likely that treatment remains beneficial. Thus, while PSMA PET-CT may be prognostic, it doesn’t necessarily change management.
For patients with high volume nodal disease, Dr. Briganti emphasized that there is no data in this space and, therefore, there is a high need for trials.
Thus, in his view, the only clinical scenario in which PSMA PET-CT would change clinical practice is one in which there are positive lymph nodes outside the template field. Based on data from Dr. Yaxley, approximately half of patients with positive lymph nodes had nodal disease outside the boundaries of lymphadenectomy. However, as Dr. Briganti highlighted, in total this represents only 4% of all patients and it is unknown whether changes in their management would actually be beneficial.
Presented by: Alexandre Ingels,1 Christopher G. Eden,2 Alberto Briganti3
- Department of Urology, Hôpital Henri Mondor, Paris France
- Department of Urology, Royal Surrey County Hospital NHS Foundation Trust, Guildford, United Kingdom
- Università Vita-Salute San Raffaele, Milan, Italy

