Dr. Mir Maresma began by highlighting the case of a 75-year-old lady who underwent a prior partial nephrectomy on the right side of a clear cell renal cell carcinoma (ccRCC) (Fuhrman grade 2) with subsequent right renal atrophy. She then was lost to follow-up and re-presented with a 7.2 cm solid, enhancing renal mass. Her baseline Cr was 1.1 (eGFR 60) with 60% renal function contributed by the left moiety. In terms of past medical history, Dr. Mir Maresma noted hypertension, obesity, and prior abdominal surgeries.
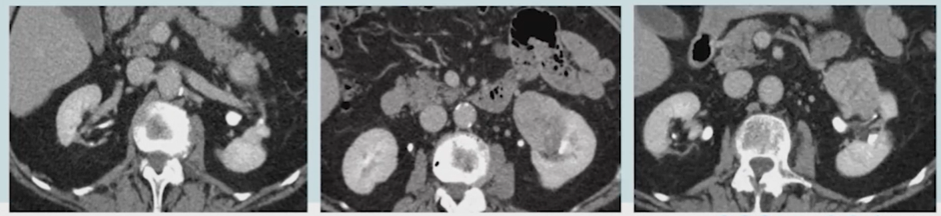
Dr. Grimm then presented on the role of radical nephrectomy in this case. He began emphasizing that radical surgery is more oncologically safe, with lower rates of complications, there is no proven benefit of kidney function in the majority of patients. He emphasized that not everything that can be done (such as partial nephrectomy), should be done.
He presented data from the EORTC 30904 trial examining kidney function and overall survival comparing partial and radical nephrectomy. Notably, this trial enrolled patients with tumors less than 5cm. Over a follow-up exceeding 9 years, partial nephrectomy was associated with worse overall survival, despite better preservation of renal function. However, the incidence of kidney failure was similar between the groups.
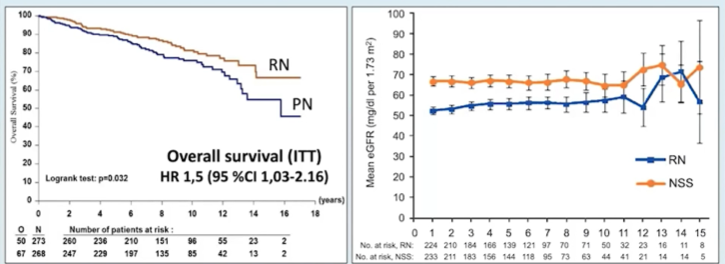
An exploratory analysis aimed to assess whether baseline differences affected the differential effect of radical vs partial nephrectomy on renal dysfunction and mortality.
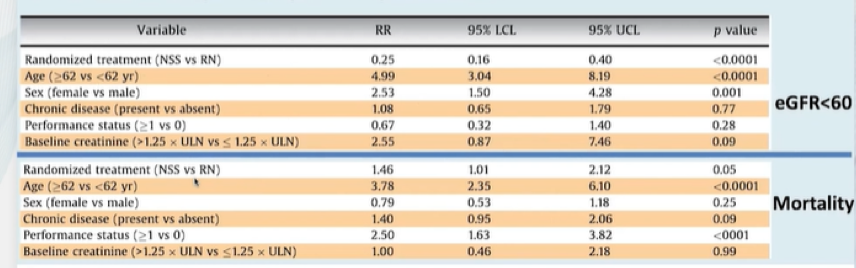
Going back to the case, Dr. Grimm emphasized that this is a moderate to high complexity tumor on the basis of PADUA score. Based on the RECORD2 data, patients undergoing partial nephrectomy for these complex masses are associated with relatively higher rates of complications and positive surgical margins (approximately 5%). More importantly, the trifecta rate (negative surgical margins, warm ischemia <25 min, and no complications) were only achieved in <50% of patients undergoing robotic-assisted partial nephrectomy and even lower among those undergoing open and laparoscopic surgery, despite most patients being treated at high volume centers.
Based on a recent systematic review comparing partial and radical nephrectomy for large renal tumors, overall complication rates and high-grade complication rates were significantly higher for patients undergoing partial nephrectomy (based on data from patients primarily treated in an open fashion). Dr. Grimm then presented data from the ROSULA Collaborative Group comparing robotic partial nephrectomy and minimally invasive radical nephrectomy in cT2a disease, demonstrating similar oncology and morbidity related outcomes. In spite of these conclusions, post-operative transfusions were more common in the partial nephrectomy group and there was twice the number of postoperative complications (including high-grade). Further, positive surgical margins were more than 3 times higher. Data from the RECOd1 project show that positive surgical margins are associated with a 7x risk of renal recurrence following partial nephrectomy.

In summary, Dr. Grimm highlighted that radical surgery does not negatively affect all-cause mortality, in spite of worse renal function preservation. Radical nephrectomy is associated with fewer complications and improved oncologic outcomes.
Dr. Minervini then presented the rationale for partial nephrectomy in patients with large RCCs (>7cm). He began by emphasizing that the guidelines recommend offering radical nephrectomy for patients with T2 tumors and those that are not treatable by partial nephrectomy.
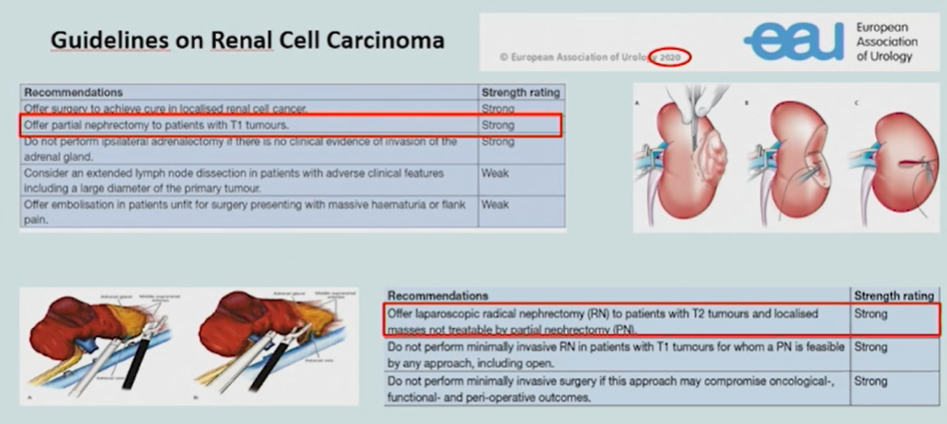
Dr. Minervini then presented data from both a recent systematic review and the ROSULA Collaborative Group highlighting that renal dysfunction is more common in patients undergoing radical nephrectomy, even in the context of cT2 disease. The systematic review, while limited by the quality of observational data included, found that new onset of chronic kidney disease and all-cause mortality was higher among patients treated with radical nephrectomy.
He then emphasized that, while tumor dimension is not a limit for nephron-sparing surgery, there are a number of circumstances that advocate for radical nephrectomy, including renal vein thrombus, renal vascular involvement, infiltrative tumor growth, and poor preservation of renal parenchyma due to the extensive resection required. In these settings, partial nephrectomy may expose patients to unnecessary perioperative risk.
For elective indications, partial nephrectomy should be considered where it does not compromise oncologic outcomes and when related benefits outweigh harms.

In contrast, there are imperative indications for nephron-sparing (including congenital, functional, or acquired solitary kidney, chronic kidney disease, and bilateral renal masses), in which nephron-sparing approaches are more strongly mandated.
When approaching partial nephrectomy for cT2 tumors, Dr. Minervini highlighted the importance of preoperative evaluation of the tumor and renal anatomy complexity, interoperative delineation of tumor anatomy, anatomic resection strategy, anatomical renorrhaphy, and use of minimally invasive approaches. Dr. Minervini highlighted the value of 3-dimensional reconstructions of the CT images to allow for better surgical planning. Further, he emphasized that intra-operative ultrasound can improve the quality of surgical resection. Dr. Minervini stressed the importance of a planned anatomic resection strategy, emphasizing the value of enucleation, particularly in these tumors.
Dr. Minervini then highlighted a number of multicenter studies showing that use of the robotic approach was protective in terms of post-operative renal function, complications, and failure to achieve the trifecta outcomes compared to both open and laparoscopic approaches. As with Dr. Grimm, Dr. Minervini highlighted the importance of both surgeon and center volume on achieving good outcomes following partial nephrectomy.
In closing, Dr. Minervini highlighted that the EAU guidelines recommend radical nephrectomy for patients with cT2 tumors, though, in his view, there remains a role for partial nephrectomy in some of these patients.
Dr. Mir Maresma then closed by sharing the outcome of the case which began this session – the patient underwent robotic partial nephrectomy with a generally uncomplicated postoperative outcome.
Presented by: Carmen Mir Maresma, MD,1 Marc-Oliver Grimm, MD,2 Andrea Minervini, MD, PhD3
- Urologic Oncology Clinical Fellow, Cleveland Clinic, Cleveland, Ohio
- Professor and Chairman, Universitätsklinikum Jena, Jena, Germany
- Professor of Urology; Department of Urology, Careggi Hospital, University of Florence, Florence, Italy

