(UroToday.com) The 2023 AUA annual meeting included a session on markers in prostate cancer, featuring a presentation by Dr. Michael Leapman discussing the association between the Decipher® genomic classifier and prostate cancer outcomes in a large-scale, real-world dataset. Although the prognostic significance of the Decipher® genomic classifier has been established in the context of randomized clinical trials and institutional cohorts, less is known about the associations between Decipher® testing and oncologic outcomes among patients treated in the real-world practice setting.
Dr. Leapman and colleagues conducted a retrospective cohort study using a novel longitudinal linkage of transcriptomic data from the Decipher® genomic classifier and real-world clinical data aggregated from insurance claims, pharmacy records, and electronic health record data across payors and sites of care. They assessed the associations between Decipher® test results and biochemical recurrence and metastasis after radical prostatectomy and prostate biopsy. Kaplan-Meier and Cox proportional hazards regression were used to examine the associations between the genomic classifier and the study outcomes adjusting for baseline clinical risk factors.
This study identified 92,976 patients who underwent Decipher® testing that were successfully linked to real-world clinical data, including 53,871 from biopsy and 39,105 from radical prostatectomy. The median age at biopsy was 68 years (IQR 62-73) and the following NCCN groupings were found:
- Low-risk: 27.3%
- Favorable-intermediate risk: 27.6%
- Unfavorable-intermediate risk: 29.8%
- High-risk: 10.8%
- Unclassified risk: 4.5%
The following box-plot illustrates the distribution of genomic classifier scores across the Gleason grade group among the entire cohort:

Among prostate biopsy patients, the genomic classifier classified 51.6%, 18.1%, and 30.3% as low, intermediate, and high risk, respectively. The following figure shows metastasis after diagnosis in biopsy tested patients:
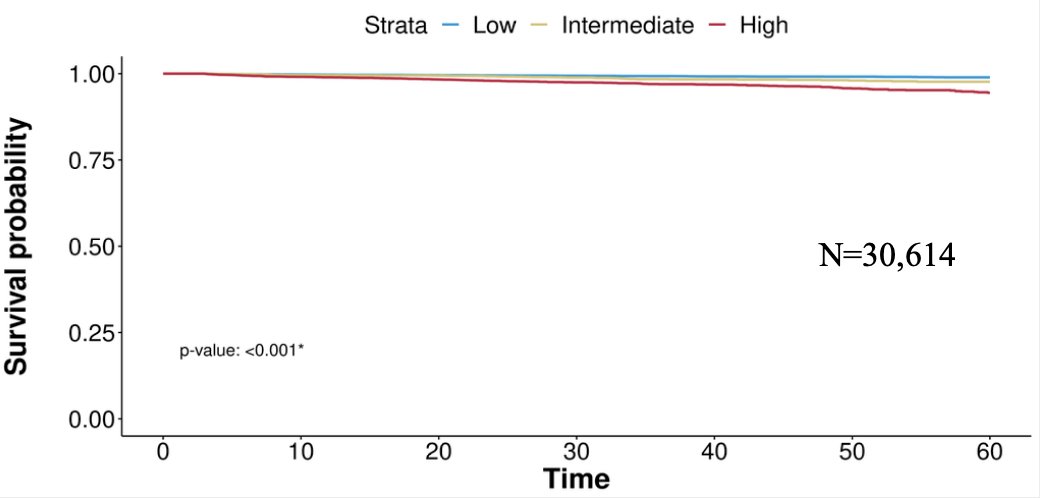
Among radical prostatectomy-tested patients, the median age was 65 years (IQR 60-69). In this subset, the genomic classifier classified 39.1%, 17.2%, and 43.7% as low, intermediate, and high risk. The BCR and metastasis after treatment in men treated with RP is as follows:
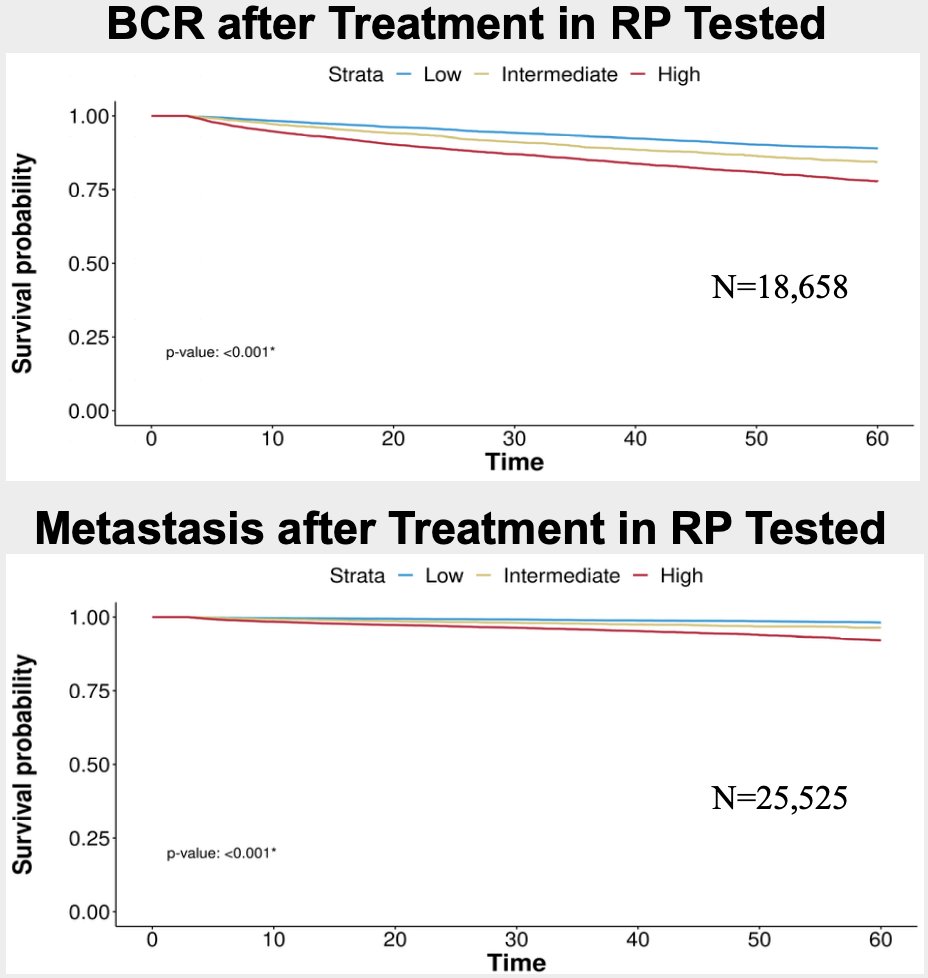
Among biopsy-tested patients, the genomic classifier was independently associated with risk of metastasis (HR 1.21 per 0.1 unit increase in genomic classifier, 95% CI 1.16-1.27, p<0.001) in models adjusted for age and NCCN risk group. Among radical prostatectomy-treated patients the genomic classifier was associated with risk of biochemical recurrence (HR 1.14 per 0.1 unit increase, 95% CI 1.12-1.16, p<0.001) and metastasis (HR 1.22 per 0.1 unit increase, 95% CI 1.19-1.26, p<0.001) in models adjusting for age and CAPRA-S.
Dr. Leapman concluded his presentation by discussing the association between the Decipher® genomic classifier and prostate cancer outcome in a large-scale real-world dataset with the following take-home messages:
- In this real-world study conducted at the national scale, Decipher® genomic classifier was independently associated with the risk of biochemical recurrence and metastasis among patients managed in contemporary practice
- These findings highlight the potential of large scale clinical-genomic linkages to enhance understanding of cancer biology estimates of treatment effectiveness
Presented by: Michael Leapman, MD, MHS, Yale University, New Haven, CT
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, @zklaassen_md on Twitter during the 2023 American Urological Association (AUA) Annual Meeting, Chicago, IL, April 27 – May 1, 2023

