In addition to comprising the focus of studies to date, clear cell RCC (ccRCC) accounts for approximately 70% of kidney cancer cases in the US. Molecular work over the past few decades has identified that a key oncogenic driver in RCC is the transcription factor hypoxia-inducible factor 2α (HIF-2α). MK-6482 is a small molecule HIF-2α inhibitor that blocks the heterodimerization of HIF-2α with HIF-1β, inducing tumor regression in mouse xenograft RCC models. In a plenary abstract presentation in the Oral Abstract Session: Renal Cell Cancer session at the 2021 ASCO GU Cancers Symposium, Dr. Todd Michael Bauer presented updated data from the first-in-human phase 1/2 study of MK-6482 in advanced solid tumors (NCT02974738).
The authors accrued patients aged 18 years and older with advanced ccRCC who had received at least 1 prior therapy, and who had evidence of measurable disease based on RECIST v1.1 criteria. Further, patients were required to have ECOG status 0 or 1, adequate organ function, and life expectancy ≥6 mo. Once accrued, patients received 120 mg of MK-6482 orally once daily, based on results from the dose-escalation cohorts.

While the primary endpoint was safety, patients were assessed at baseline, within 7 days before week 9, and then every 8 weeks with response assessed using RECIST v1.1 with key secondary end points included ORR, duration of response (DOR), and PFS.
Fifty-five patients with ccRCC were treated with MK-6482 120 mg (52 in expansion and 3 in dose-escalation cohorts). Patients had received a median number of 3 (range 1-9) prior lines of therapy. Forty-two patients (81%) previously received PD-1/L1 inhibitors and 48 (92%) previously received VEGF inhibitors. According to IMDC criteria, 13 patients (24%) had favorable risk and 42 (76%) had intermediate or poor-risk disease.
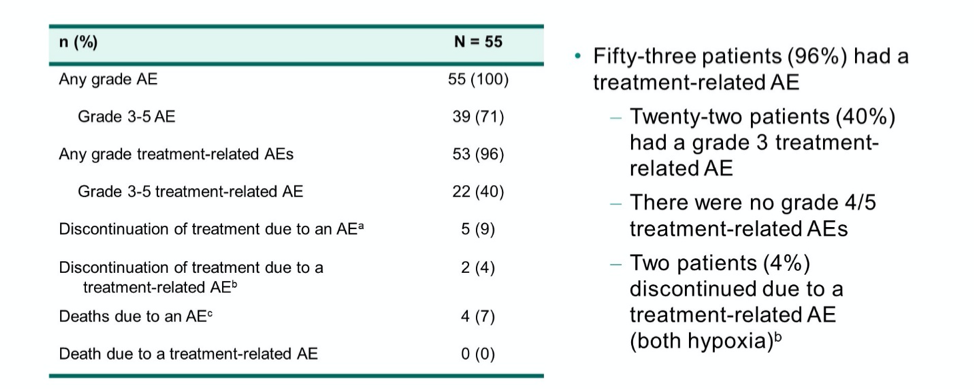
Over a median follow-up of 28 months, the most common all-grade, all-cause adverse events which were experiences in at least 30% of patients were anemia (76%), fatigue (71%), dyspnea (49%), nausea (36%), cough (31%), and hypoxia (31%). In terms of grade 3 adverse events, anemia (27%) and hypoxia (16%) were the most common. Grade 4 adverse events were experienced by two patients (4%) while 4 patients (7%) experienced grade 5 adverse events; however, no grade 4 or 5 AEs were related to treatment.

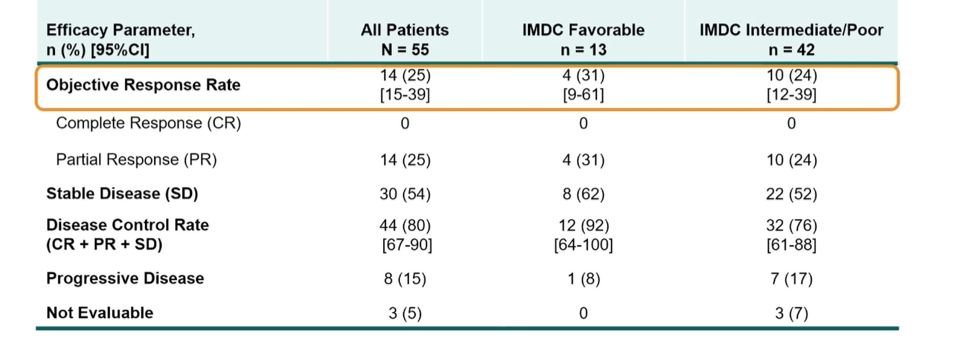
The objective response rate (ORR) was 25%, with 14 patients having confirmed PRs, and 30 patients (55%) having stable disease. Thus, the disease control rate (CR+PR+SD) was 80% with a median DOR that was not reached (77% had a response of at least 6 months).
Stratified by IMDC risk, 4 of 13 patients with favorable risk had PR (ORR = 31%) and 10 of 42 with intermediate or poor risk had PR (ORR = 24%) with corresponding disease control rates of 92% and 76%, respectively.
In the overall population, median PFS was 14.5 months with 1-year progression-free survival of 51%.
As of June 1, 2020, 33 patients (60%) discontinued because of PD and 2 (4%) because of AEs while 11 patients (20%) had ongoing treatment.
Dr. Bauer thus concluded that MK-6482 demonstrates promising single-agent activity in patients with ccRCC and warrants assessment in a phase III trial which is underway.
Presented by: Todd Michael Bauer, MD, Medical Oncology, Tennessee Oncology
Written by: Christopher J.D. Wallis, Urologic Oncology Fellow, Vanderbilt University Medical Center Contact: @WallisCJD on Twitter during the 2021 American Society of Clinical Oncology Genitourinary Cancers Symposium (#GU21), February 11th-February 13th, 2021

