For this study, the authors queried a multi-institutional database for patients diagnosed with urothelial carcinoma between 2008-2018 in five Southeastern Pennsylvania counties (Montgomery, Chester, Delaware, Philadelphia, and Bucks county) which has a population of ~4 million people and a yearly incidence of urothelial carcinoma of ~1,000 cases:
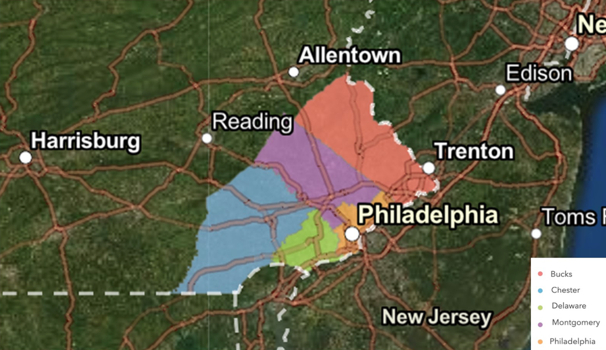
Inclusion criteria included patients >40 years of age and a diagnosis of urothelial carcinoma from ICD 9/10 codes (renal pelvis/calyces, ureters, bladder, urethra; n=9,009). Patients were excluded if they were diagnosed prior to 2008 or after 2018, were inaccurately coded, had non-urothelial histology, resided beyond any of the five noted counties, or had incomplete address information. Socioeconomic factors included median income and educational attainment, and demographic factors included age, sex, ethnicity, industrial/occupational exposure. Clinicopathologic factors included alcohol use, tobacco use, comorbidities, and cancer diagnosis (site, stage, grade, variant histology), and environmental risk factors included discharge of industrial byproducts (from the Pennsylvania and US Environmental Protection Agencies), and vehicle-related organic compound emissions (planes, automobiles – sources: Pennsylvania Department of Transportation and Federal Aviation Administration).
Geocoded addresses and ArcGIS software were used to calculate the Getis-Ord-Gi* statistic and perform hotspot analysis on the census-block level to identify urothelial carcinoma hotspots. Demographics, clinicopathologic disease characteristics, and proximity to sources of industrial byproducts and environmental pollutants were compared using Pearson’s chi-square and Student’s T-test. Univariate analyses and multivariable multilevel logistic random-intercept regression models were fitted to test the association between patient and census block-level factors and living in a urothelial carcinoma hot spot.
Among 5,080 patients meeting inclusion/exclusion criteria, 148 patients (2.9%) were associated with one of three urothelial carcinoma hotspots:
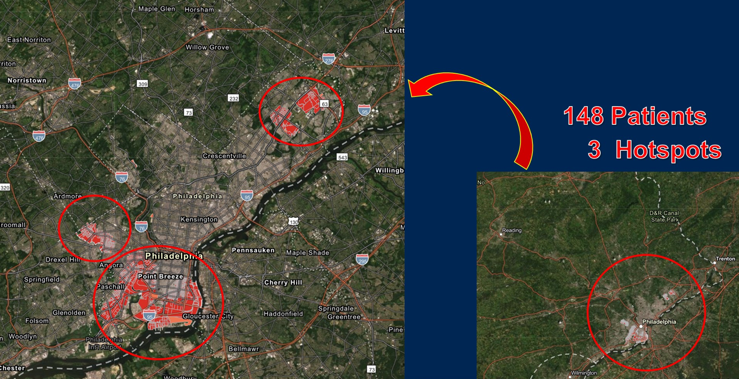
In univariate analyses, hotspot patients were less likely to be tobacco users (OR 0.24, p=0.004) or of white race (OR 0.10, p<0.001) and less likely to have higher income (OR 0.73, p=0.005). They were more likely to be associated with industrial byproducts and environmental pollutants exposure (OR 8.24, p=0.001). Multivariable analysis confirmed increased likelihood of residing in a urothelial carcinoma hotspot and proximity to high-traffic density (OR >999, p < 0.001) and sites of industrial byproducts and environmental pollutants contamination (OR 48, p < 0.009), with decreased likelihood of tobacco use (OR 0.39, p=0.031) and non-white race (OR 16.7, p < 0.001).
Several limitations of this study provided by Dr. Edwards included: (i) retrospective design, (ii) despite a large sample size, this study only represented ~50% incidence of urothelial carcinoma, (iii) though multiregional, referral patterns may affect the population, (iv) difficult to assess timing and duration of exposure, (v) proximity to the source may not necessarily represent a surrogate for exposure, and (vi) prospective research with increased granularity will better define risk.
Dr. Edwards concluded with the following take away messages:
- Spatially-related clusters of urothelial carcinoma may be associated with locoregional environmental exposures
- Patients residing within urothelial carcinoma hotspots may be more likely to be less-educated, lower-earning, of non-white race, and women
Presented by: Daniel C. Edwards, DO, Urologist, Levine Cancer Institute at Atrium Health, Charlotte, NC
Written by: Zachary Klaassen, MD, MSc – Urologic Oncologist, Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia Twitter: @zklaassen_md during the 2021 American Society of Clinical Oncology Genitourinary Cancers Symposium (#GU21), February 11th-February 13th, 2021
