(UroToday.com) At the 2022 American Society of Clinical Oncology Annual Meeting held in Chicago and virtually, the poster session focused on Prostate, Testicular, and Penile cancers on Monday afternoon included a presentation from Dr. Nishwant Swami describing disparities in diagnosis, access to treatment, and treatment delays for Hispanic men with metastatic prostate cancer.
Dr. Swami noted that there is significant heterogeneity in the social determinants of health among subgroups of Hispanic men. Thus, aggregate reporting of racial/ethnic disparities may obscure important differences. To better address this, the authors sought to identify differences in delayed diagnosis, treatment status, and time to treatment among Hispanic subpopulations with metastatic prostate cancer.
To do this, they used data from the National Cancer Database (NCDB) between 2004 and 2017 to identify patients with prostate adenocarcinoma. Patients were categorized by racial subgroup and Hispanic country-of-origin. Ordinal logistic regression was used to calculate the adjusted odds ratios (aORs) with associated 95% confidence intervals for the following disparity related outcomes:
- the likelihood of presenting with Stage IV cancer;
- the likelihood of receiving treatment; and
- the likelihood of receiving delayed treatment. This was defined in the primary analysis as a treatment after 90 days though was varied to 180 days in a sensitivity analysis.
They found that, among 1,305,785 patients, Hispanic men had greater odds of presenting with stage IV prostate cancer compared with non-Hispanic White (NHW) men (aOR = 1.54 95% CI 1.50-1.58, p < 0.001). Further, this effect was observed across all Hispanic racial subgroups, though the highest odds were observed in Hispanic Black men (aOR 1.68 95% CI 1.46-1.93, p < 0.001). Disparities were also observed in all country of origin subgroups, particularly for men of Mexican heritage (aOR 1.99 95% CI 1.86-2.12, p < 0.001).
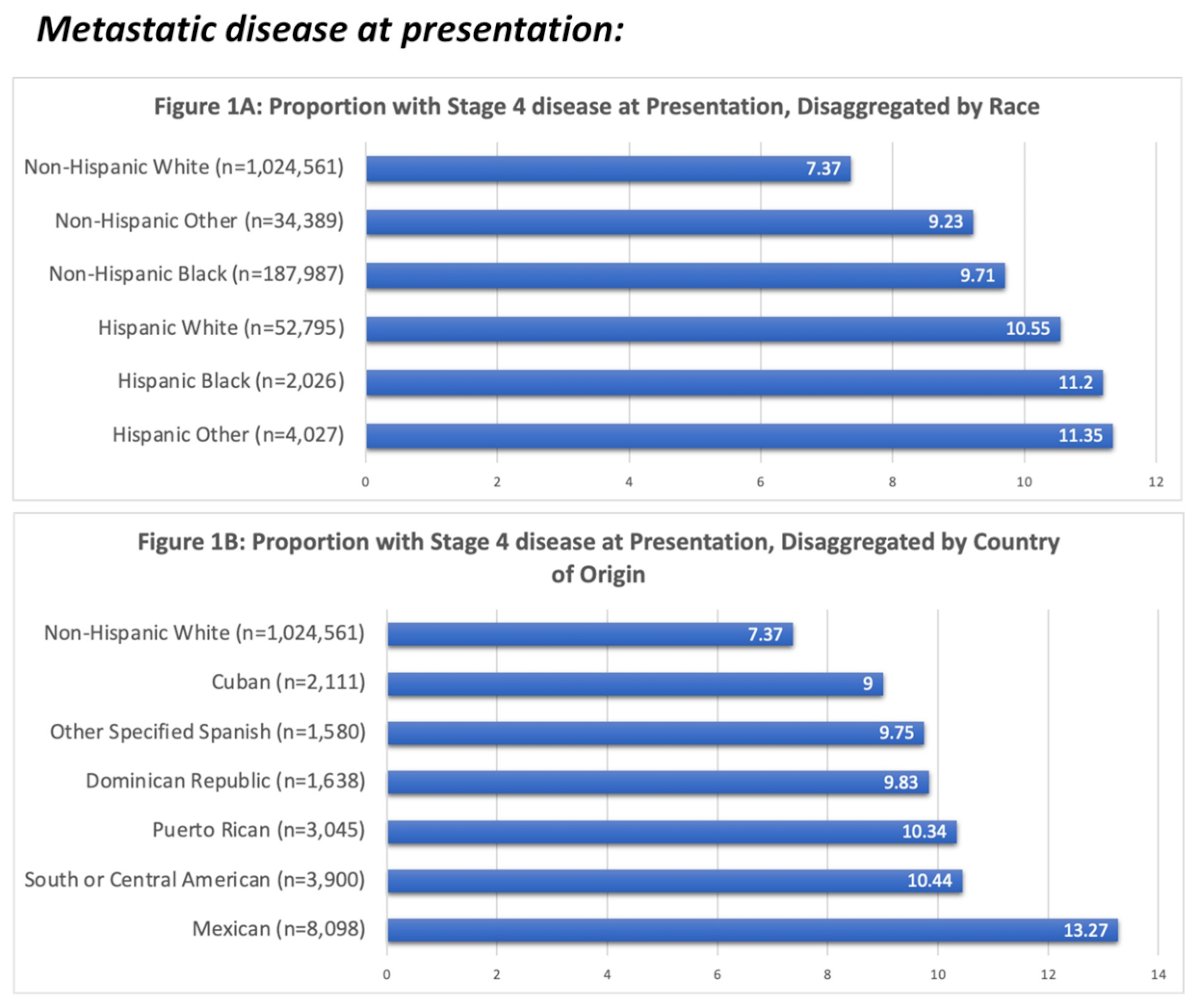
Among men with metastatic disease, Hispanic men were less likely to receive treatment than NHW men (aOR 0.60 95% CI 0.53-0.67, p < 0.001). Hispanic White patients were less likely to receive treatment compared with NHW men (Hispanic White aOR 0.58 95% CI 0.52-0.66, p < 0.001). Upon disaggregation by country of origin, disparities persisted, particularly for men of Dominican heritage (aOR 0.52 95%CI 0.28-0.98 p = 0.044).

Finally, Hispanic men were more likely to experience treatment delays when compared to NHW men (aOR 1.38 95%CI 1.26-1.52 p < 0.001). All Hispanic racial subgroups experienced greater treatment delays, particularly Hispanic Black men (aOR 1.83 95%CI 1.22-2.75 p = 0.002). Men of Central or South American heritage had the greatest odds of treatment delays (aOR 1.48 95%CI 1.07-2.04 p = 0.018). Sensitivity analysis indicated consistent findings among Hispanic patients overall, Hispanic White patients, and patients of Mexican and Puerto Rican heritage.
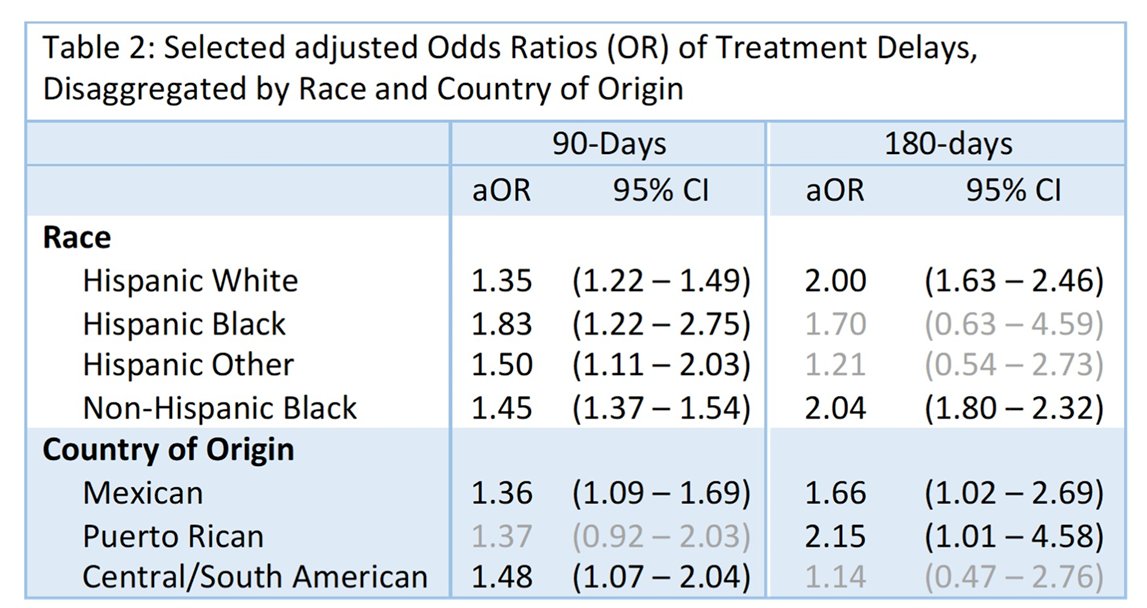
Thus, in conclusion, the authors demonstrate notable disparities in prostate cancer diagnosis and treatment for Hispanic men, with meaningful differences when stratified by racial subgroup and Hispanic country of origin.
Presented by: Nishwant Swami, MPH, University of Massachusetts Medical School, Worcester, MA

